WHO flags global case cluster, but says risk remains low — NCDC on alert as hantavirus travel-linked cluster widens — Why Nigeria is watching a virus it has not yet recorded
By Nkanu Egbe
Three passengers are dead. Eight cases have been confirmed or suspected across multiple countries. A Dutch-flagged cruise ship carrying 147 passengers and crew is navigating its way toward the Canary Islands under the watchful eyes of health ministries from more than 22 nations. And in Abuja, the Nigeria Centre for Disease Control and Prevention has issued a public health advisory about a disease it has never officially recorded in this country.
This is the hantavirus episode of May 2026 — and it is less about an unfolding Nigerian epidemic than it is a test of whether public health early-warning systems can move faster than a virus can travel. The tension between “low risk” and “high alert” is precisely what makes this story worth following.
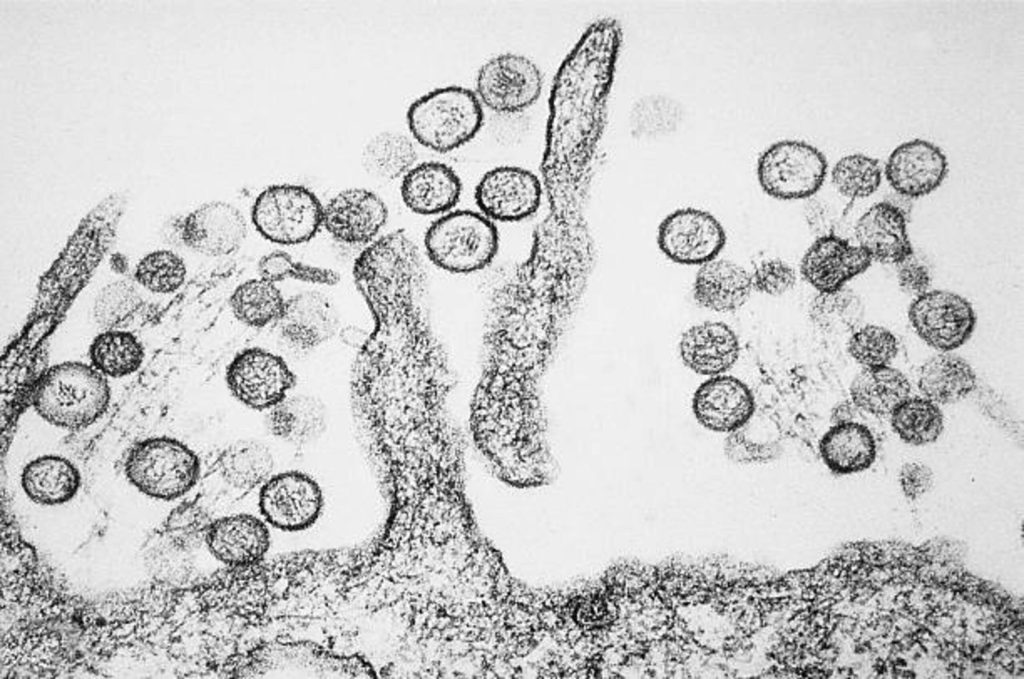
What Happened: A Cruise Ship, a Rare Virus, and Three Deaths
The sequence of events began quietly. On April 6, a Dutch passenger aboard the MV Hondius — a Dutch-flagged expedition vessel that had departed Ushuaia, Argentina on April 1 — fell ill with fever and symptoms resembling pneumonia. He died five days later. Because his presentation resembled other respiratory illnesses, hantavirus was not initially suspected, and no diagnostic samples were taken.
His wife, a 69-year-old woman who had travelled with him through Argentina, Chile, and Uruguay before boarding the ship, disembarked when the vessel docked at Saint Helena — a remote British island territory in the South Atlantic — on April 24. She deteriorated during a flight to Johannesburg and died on arrival on April 26. Laboratory testing later confirmed the Andes strain of hantavirus infection in her blood.
A third passenger died on board. By the time WHO issued its disease outbreak notice on May 4, seven cases had been identified — two confirmed and five suspected — with three deaths. As of today, May 9, the WHO reports eight cases total, six of which have been laboratory-confirmed, still with three fatalities.
WHO Director-General Tedros Adhanom Ghebreyesus, addressing reporters this week, was direct: “While this is a serious incident, WHO assesses the public health risk as low.” But he also acknowledged something that has complicated that reassurance considerably — the hantavirus strain involved, the Andes virus, is the only known hantavirus capable of limited human-to-human transmission. And given an incubation period of up to six weeks, the WHO warned that more cases could still emerge from passengers who had already disembarked.
The scale of the international response underlines just how seriously authorities are treating the event even as they counsel against panic. Spain is coordinating the ship’s arrival in Tenerife with 22 countries and the WHO. Almost all countries with nationals on board are sending evacuation aircraft. The WHO’s director-general has personally travelled to Tenerife for the disembarkation. Passengers are currently hospitalised in South Africa, the Netherlands, Germany, Saint Helena, Spain, and Switzerland.
Nigeria’s Response: No Cases, But Heightened Watch
For Nigeria, the starting point is reassuring. The NCDC, in a public health advisory issued on Friday and signed by Director-General Dr. Jide Idris, was unequivocal: there is currently no confirmed or suspected hantavirus case anywhere in the country.
“At this time, there is no evidence of hantavirus cases in Nigeria,” the advisory stated. “NCDC is closely monitoring the situation and maintaining surveillance for emerging infectious diseases.”
The agency has activated heightened surveillance measures and has committed to tracking global developments through its systems for epidemic-prone and emerging infectious diseases. That institutional posture — watchful rather than alarmed — is the appropriate response given what the evidence currently shows.
Dr. Idris acknowledged that the current cluster is linked to the Andes virus strain, which has previously demonstrated limited human-to-human transmission, particularly through close contact such as between household members, intimate partners, or healthcare workers. The NCDC’s advisory also emphasised the importance of practical hygiene measures: keeping environments clean, preventing rodent infestation, storing food properly, and avoiding contact with rodents or their droppings.
Nigeria has not appeared on any list of countries with nationals who were aboard or connected to the MV Hondius. The ship’s route — from Argentina through the South Atlantic to Saint Helena, Ascension Island, Cape Verde, and now toward the Canary Islands — does not intersect directly with Nigerian ports. But the NCDC’s decision to issue an advisory is not reflexive caution. It reflects an understanding that in a country with major international airports, significant port traffic, and active diaspora travel networks, the lag between a global health event and a potential domestic case can be shorter than anyone expects.
What Hantavirus Is: Rodent-Borne, Rarely Human-to-Human
For Lagos readers encountering the name hantavirus for the first time, a brief explanation is useful. Hantaviruses are a family of more than fifty viral strains, all carried primarily by rodents. Humans become infected not through rodent bites, but through contact with infected rodent urine, droppings, saliva, or dust contaminated by those materials — typically during cleaning of rodent-infested spaces without adequate protection.
The clinical picture is serious. Symptoms begin with fever, fatigue, body aches, and gastrointestinal complaints, and can progress rapidly to pneumonia, acute respiratory distress syndrome, and in severe cases, circulatory collapse. The case fatality rate varies significantly by strain — under one percent to fifteen percent for strains common in Asia and Europe, and as high as fifty percent for strains circulating in the Americas.
The Andes virus, identified in the MV Hondius outbreak, is found primarily in South America. It carries the distinction of being the only hantavirus strain known to spread from person to person, though previous outbreaks show this transmission is uncommon and requires prolonged, close contact. A 2018 outbreak in the Argentine village of Epuyen, which infected 34 people and killed 11, offers the most documented precedent. It is that outbreak — and the Andes virus’s unusual person-to-person capacity — that explains why WHO is more concerned about this cluster than a standard environmental hantavirus exposure would warrant.
Globally, hantavirus infections remain rare. In 2025, the Americas recorded 229 cases and 59 deaths across eight countries. Argentina, where the likely exposure of the Dutch index case occurred during a birdwatching trip that may have brought him into contact with a landfill used by infected rodents, has seen cases rise sharply since mid-2025 — from 28 deaths to 101 confirmed infections since June 2025, roughly double the previous year’s figures.
Why the Risk Is Still Relevant for Lagos
Low global risk does not dissolve local concern — and for a city of Lagos’s scale, the variables that matter are specific.
Lagos is home to one of Africa’s busiest international airports. Murtala Muhammed International Airport handles tens of millions of passengers annually, connecting the city to destinations across South America, Europe, and beyond. Tin Can Island and Apapa ports process substantial cargo and personnel traffic. Lagos Island and the mainland together constitute one of the world’s largest urban agglomerations, where rodent populations share space with millions of residents across a range of sanitary conditions.
None of these factors create an imminent hantavirus threat. But they are precisely the conditions under which an imported case — arriving via a traveller who picked up an infection before symptoms appeared — could go undetected for days before the respiratory deterioration signals something unusual. The hantavirus incubation period of up to six weeks means that someone exposed in Argentina on April 1 might not show symptoms until mid-May. Clinicians unfamiliar with the disease could plausibly misread early symptoms as typhoid, COVID-19 complications, or any number of more common respiratory presentations.
That diagnostic gap is one reason the WHO is maintaining what amounts to a global lookout even as it downplays pandemic risk. It is also why the NCDC’s decision to enhance surveillance now — before any case arrives — is the correct call. Early-warning systems are most valuable precisely when there is still nothing to warn about.
Public Health Takeaways: Vigilance Without Panic
Neither the WHO nor the NCDC is recommending travel restrictions. No advisory urges Nigerians to avoid any particular destination. The practical guidance from both agencies is consistent and mundane in the best sense: environmental hygiene, rodent control, prompt reporting of unexplained respiratory illness, and reliance on verified information from official sources.
For healthcare providers in Lagos, the advisory carries an implicit professional instruction: if a patient presents with fever and rapid respiratory deterioration, and has a travel history involving South America or contact with someone who has, hantavirus should enter the differential diagnosis even if it seems unlikely. Early supportive care — the only treatment available, since there is no licensed specific antiviral or vaccine for hantavirus — can significantly improve outcomes if applied early enough.
For the general public, the message is simpler. Hantavirus is a disease of rodent exposure. Urban Nigerians who avoid close contact with rodents, keep their environments clean, and dispose of waste properly are already practising the primary preventive behaviour that applies here. That is not reassurance for reassurance’s sake. It reflects how the disease actually works.
A Test of Early Warning, Not a Sign of an Epidemic
The hantavirus episode of May 2026 will most likely be recorded as a tragic but contained cluster — a cruise ship outbreak with three deaths, significant international disruption, and no wider epidemic. WHO’s assessment of low public health risk is well-grounded in the epidemiology of the Andes virus: difficult to transmit, requiring sustained close contact, with no historical precedent for large-scale community spread outside a clustered exposure event.
But the episode also reveals something important about how public health systems must behave in an era of rapid international travel. The NCDC did not wait for a case to arrive before issuing guidance. WHO did not wait for pandemic-level spread before coordinating a 22-nation evacuation. The Spanish health ministry did not wait for the ship to dock before establishing isolation protocols. These responses are not overreactions. They are what a functioning early-warning system looks like in practice.
For Lagos, the hantavirus alert is not a sign of an approaching crisis. It is a reminder that the gap between “no cases here” and “cases here” can close faster than surveillance systems can catch up — and that the time to prepare is before that gap closes, not after.


